You’ve had your wisdom teeth out. The procedure went smoothly, you made it home, and now you’re sitting there with an ice pack on your face wondering: is this much swelling normal, and when is it actually going to go away?
First — if you’re reading this in the hours after your extraction, you’re in the right place. Swelling after wisdom tooth removal is one of the most predictable parts of the recovery, and understanding what to expect (and when it should improve) makes the whole experience far less stressful.
This guide walks you through everything: what causes the swelling, a day-by-day timeline of what to expect, the difference between normal healing and warning signs, and practical steps to help your recovery go as smoothly as possible.
If you’re concerned about your recovery and you’re a patient of Karrinyup Dental Centre, please don’t hesitate to contact us directly — that’s what we’re here for.
Disclaimer: Individual recovery varies. The information in this article is general guidance. If swelling is worsening after day three, or you develop fever, difficulty breathing or swallowing, please contact Karrinyup Dental Centre or seek urgent medical attention.
Contents Navigation
- What Causes Swelling After Wisdom Teeth Removal?
- Typical Swelling Timeline: A Day-by-Day Guide
- What’s Normal vs What’s a Warning Sign
- How to Reduce Swelling Faster: Practical Tips
- Foods That Help vs Foods That Make Swelling Worse
- When to Contact Karrinyup Dental Centre About Your Swelling
- Frequently Asked Questions
- Concerned About Your Recovery? We’re Here.
- Sources
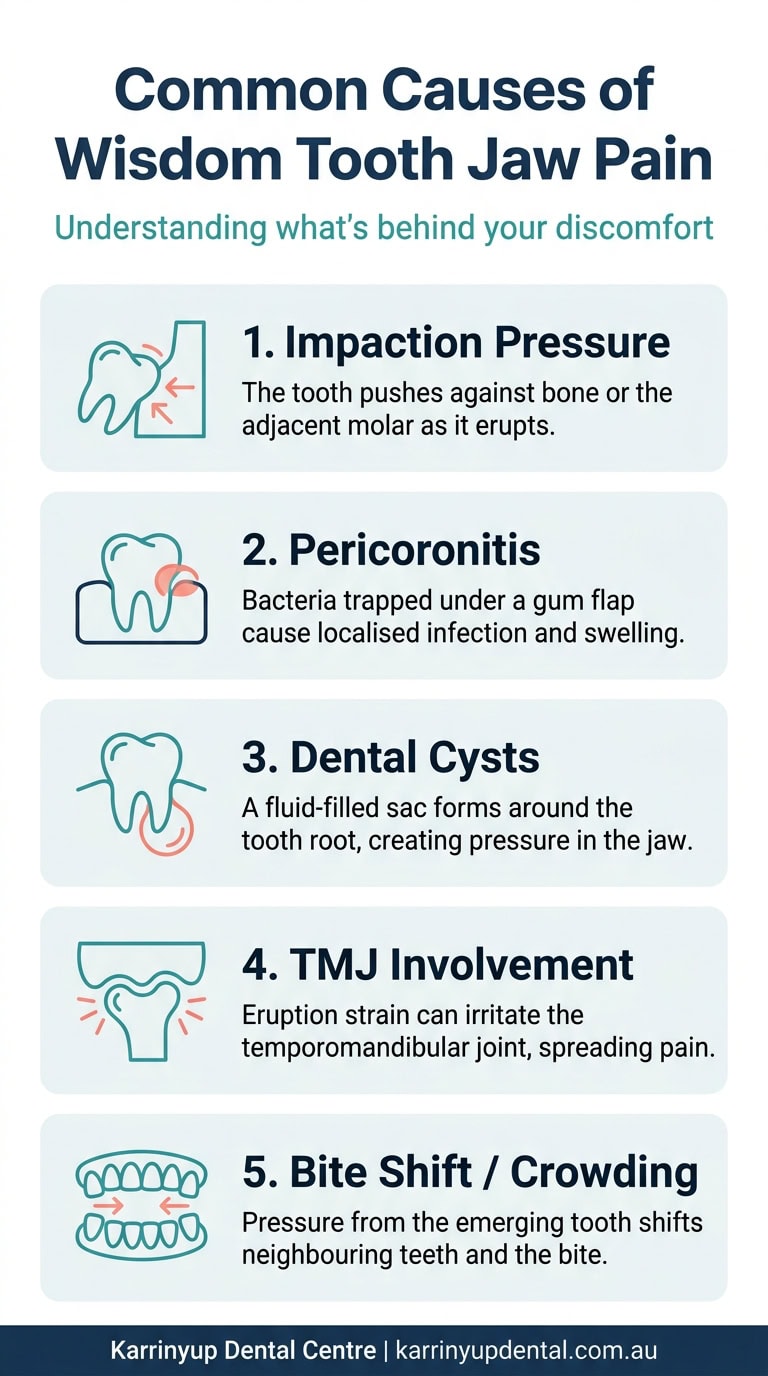
What Causes Swelling After Wisdom Teeth Removal?
Swelling after an extraction isn’t a sign that something went wrong. It’s your body’s completely normal inflammatory response to a surgical procedure.
When a wisdom tooth is removed — particularly an impacted one — the surrounding bone, gum tissue, and blood vessels are disturbed. The body immediately begins its healing response by increasing blood flow to the area and sending specialised cells to start the repair process. That increased blood flow and fluid accumulation in the tissue is what causes the characteristic puffiness in the jaw and cheek.
The degree of swelling varies significantly between patients and is influenced by several factors:
Complexity of the extraction: A fully erupted wisdom tooth that comes out cleanly typically produces less post-operative swelling than an impacted tooth that required surgical access, bone removal, or sectioning. More surgical disturbance = more tissue response.
Individual healing biology: Some patients swell dramatically after minor dental procedures. Others have a relatively minor extraction and barely swell at all. This variation is genuine and not fully predictable.
Position of the tooth: Lower wisdom teeth tend to produce more noticeable swelling than upper ones, because the lower jaw has less room for fluid dispersal and the muscles in the area are closer to the surface.
Pre-existing infection: If pericoronitis (gum infection around the wisdom tooth) was present before the extraction, there may be more soft tissue inflammation involved, and swelling can take slightly longer to fully resolve.
Post-operative care: How well you follow the post-operative instructions — particularly in the first 24 hours — has a real influence on how much you swell and how quickly it settles.
Typical Swelling Timeline: A Day-by-Day Guide
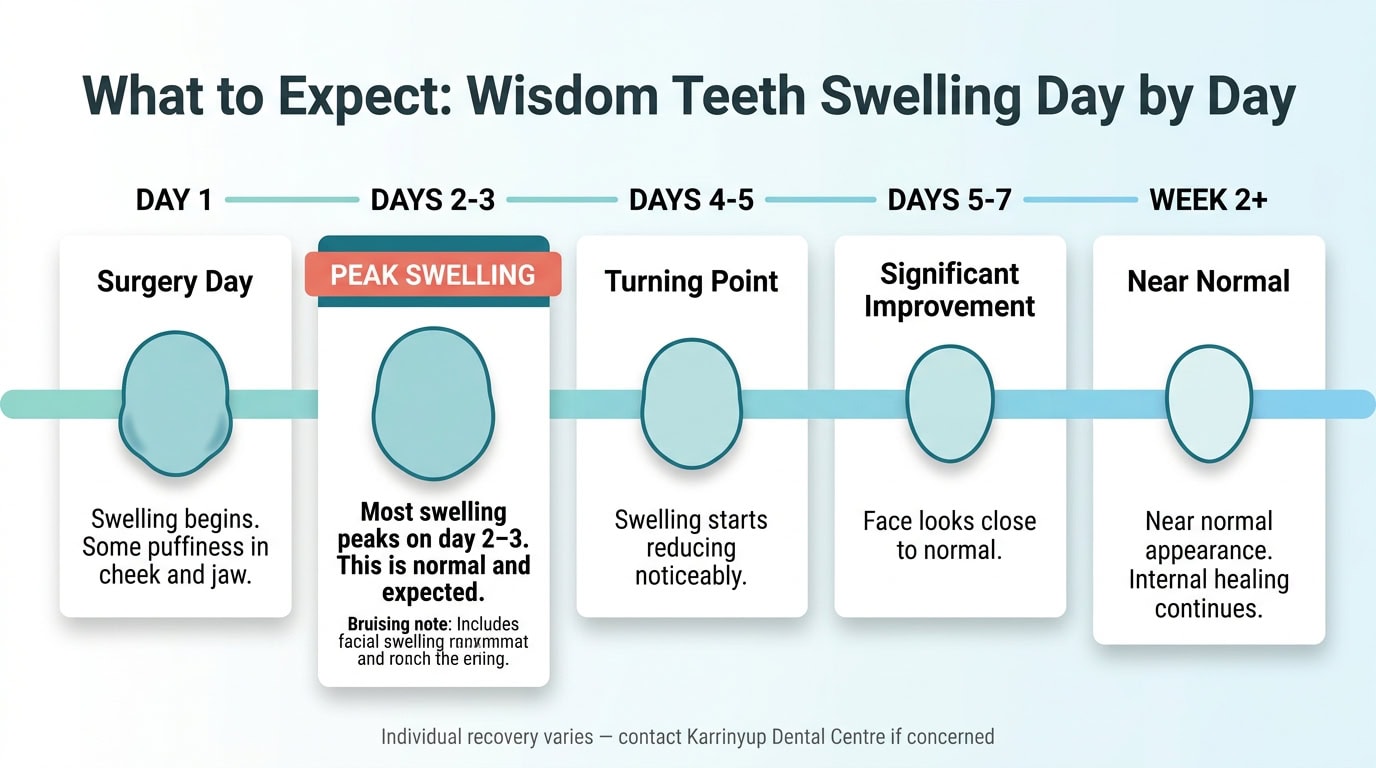
Understanding the expected arc of swelling helps you know whether you’re on track.
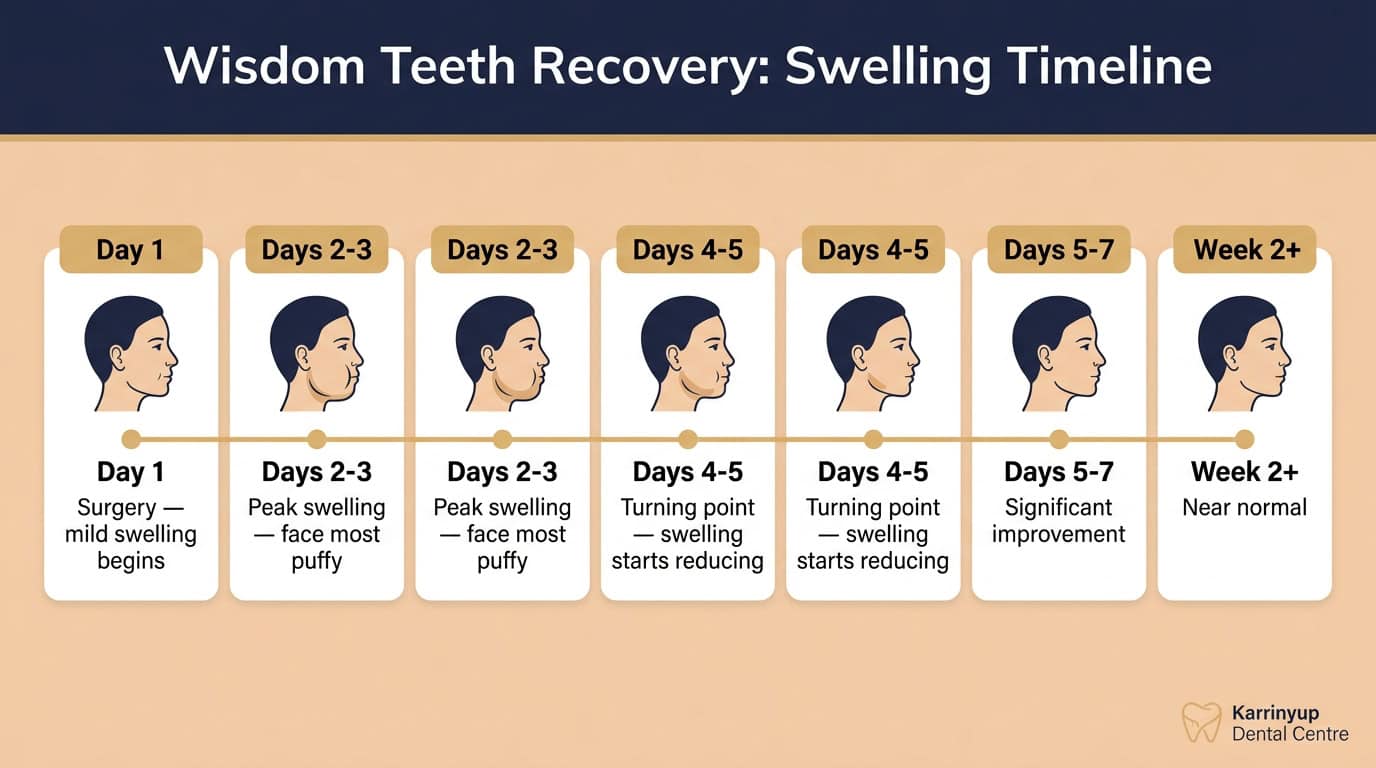
Day 1 — The Day of Surgery
Swelling after wisdom tooth extraction almost always starts within a few hours of the procedure. By the end of the first day, you’ll likely notice puffiness in the cheek, jaw, and possibly under the eye on the side where the tooth was removed.
This is expected. The tissue is reacting to the surgery, and the anaesthetic is wearing off during this period.
Key actions on Day 1:
- Apply a cold pack (wrapped in a cloth) to the outside of the cheek — 20 minutes on, 20 minutes off. Cold is effective at reducing swelling during this phase.
- Keep your head elevated — even while resting. Prop up with an extra pillow so your head is above your heart.
- Avoid any activity that increases blood pressure or blood flow to the face (exercise, bending over, heavy lifting).
- Follow any prescribed medication schedule from your dentist.
Bleeding is also common on Day 1. Some oozing of blood-tinged saliva is normal. Bite firmly on the gauze as directed.
Days 2–3 — Peak Swelling
Here’s the stage that catches many patients off guard: swelling typically peaks around 48 to 72 hours after the extraction, not immediately after. If you woke up on Day 2 and thought this looks worse than yesterday — that’s normal.
The bruising, if any, also often becomes more visible during this period. Bruising on the jaw, neck, or even the chest is a normal physiological response as old blood disperses through the tissue. It can look alarming but is not a cause for concern on its own.
What to do at peak swelling:
- Continue pain management as directed. Over-the-counter anti-inflammatories remain effective at this stage.
- Switch from cold packs to warm packs if it’s past 48 hours from surgery — warmth promotes blood flow and helps resolve the swelling more quickly at this later stage.
- Eat soft, nutritious foods. Keep your fluid intake up.
- Rest. Physical exertion slows healing.
- Avoid the extraction site with your tongue or fingers — the blood clot forming in the socket is protecting the underlying bone. Disturbing it risks dry socket.
Days 4–5 — The Turning Point
For most patients, Day 4 brings a noticeable shift. Swelling begins to reduce and the pain that required regular medication may now be manageable with occasional relief only, or none at all.
This is the stage where many patients feel well enough to consider returning to light activities — though we recommend listening to your body and not rushing back too quickly.
If your swelling is still clearly increasing on Day 4 or 5, or if you’ve developed a fever alongside the swelling, please contact us. Increasing swelling at this stage can indicate a developing infection that may need assessment.
Days 5–7 — Significant Improvement
Most patients see dramatic improvement during Days 5–7. The jaw typically looks close to normal from a distance, though you may still feel some firmness or tenderness when pressing on the area. Any visible bruising may still be working its way through the skin — this is normal.
Most people return to work, social activities, and a more normal diet during this period, depending on the nature of their job and the complexity of their extraction.
Week 2 and Beyond — Near Normal
By the end of the second week, most patients feel fully recovered from their extraction. The extraction socket is still healing internally — bone fills in over the following weeks to months — but externally, swelling, bruising, and discomfort are typically resolved.
Some patients notice mild firmness or sensitivity at the extraction site for several weeks, which is part of normal tissue remodelling. This is generally not concerning unless accompanied by new or worsening pain.
What’s Normal vs What’s a Warning Sign
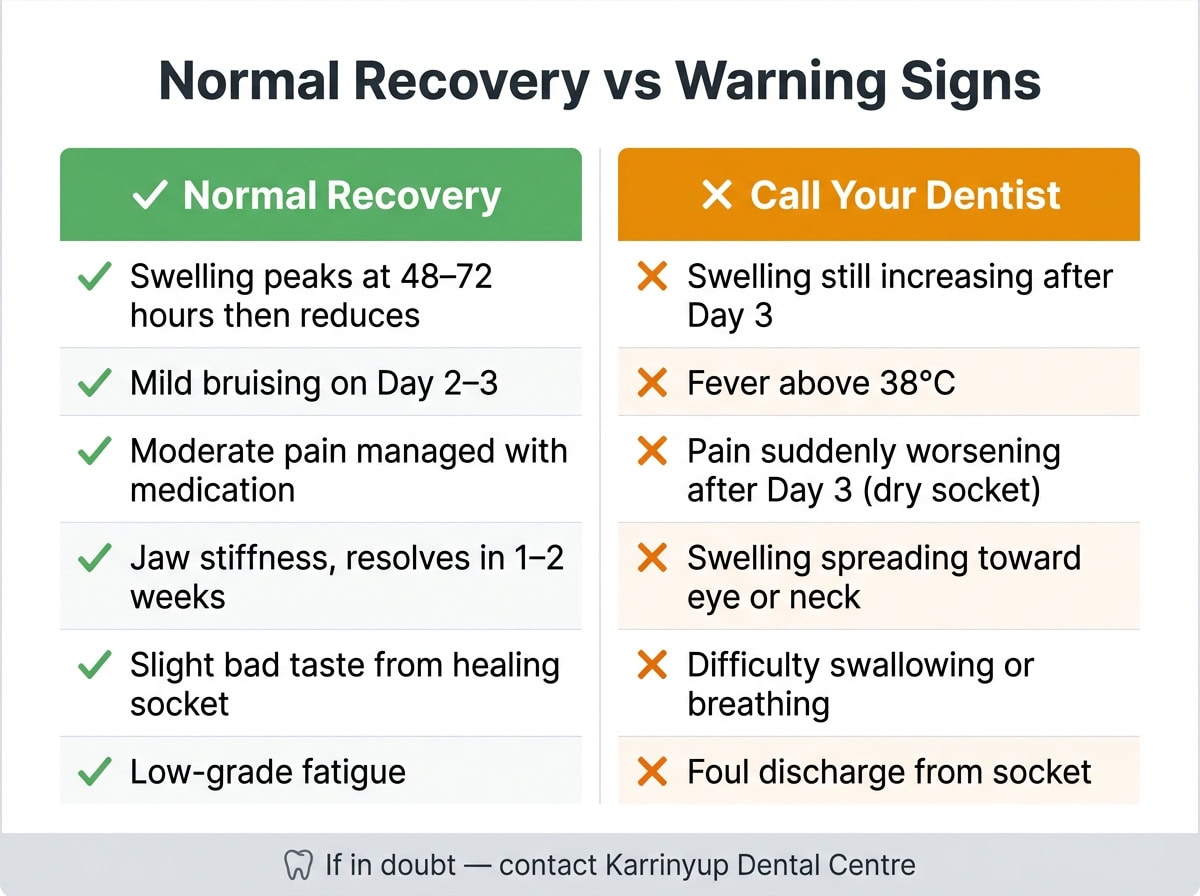
Knowing when to call your dentist versus when to wait is one of the most practically useful things we can tell you.
Normal Recovery Symptoms
- Swelling that peaks at 48–72 hours and then gradually decreases
- Bruising that develops on Day 2–3 and fades over the following week
- Mild to moderate pain, managed with over-the-counter medication
- Jaw stiffness or difficulty opening widely (known as trismus) — typically resolves within 1–2 weeks
- Slight bad taste from the healing socket — common as the clot matures
- Sensitivity at the extraction site when eating or drinking during the first week
- Low-grade fatigue — the body is doing significant repair work
Symptoms That Warrant a Call to Karrinyup Dental Centre
Dry socket (alveolar osteitis):
Dry socket is the most common complication after wisdom tooth extraction, affecting a small percentage of patients (more common in lower extractions and in smokers). It occurs when the protective blood clot that forms in the socket is dislodged or dissolves before the underlying bone has healed.
Signs of dry socket include:
- Pain that worsens significantly between Days 3–5 rather than improving
- A throbbing, radiating pain that extends into the jaw, ear, or temple
- A visible empty-looking socket with no dark blood clot
- A bad smell or taste from the socket that wasn’t present earlier
Dry socket is not dangerous but is genuinely painful. It responds well to professional treatment — we clean the socket and place a soothing dressing that provides rapid relief for most patients. Please don’t try to manage this at home.
Post-operative infection:
Symptoms of a developing infection include:
- Swelling that is increasing rather than decreasing after Day 3
- Fever (temperature above 38°C)
- Increasing redness and warmth around the extraction site
- Foul-tasting discharge from the socket
- Feeling generally unwell alongside localised symptoms
Seek urgent care if you experience:
- Swelling spreading toward the eye socket, neck, or floor of the mouth
- Difficulty swallowing or breathing
- High fever alongside jaw pain and swelling
- Significant trismus (inability to open your mouth at all)
These are signs of a spreading infection that requires prompt medical attention — beyond a routine dental review.
How to Reduce Swelling Faster: Practical Tips
There’s no way to completely bypass your body’s healing response, but you can influence how significant the swelling becomes and how quickly it resolves.
Cold in the first 24–48 hours:
Apply an ice pack (or bag of frozen peas) wrapped in a cloth to the outside of the cheek. Cold constricts blood vessels and reduces fluid accumulation. Use 20-minutes-on, 20-minutes-off during waking hours for the first day or two.
Warmth from 48 hours onward:
Once swelling has peaked, gentle warmth (a warm face cloth or heat pack) promotes circulation and helps clear the accumulated fluid from the tissue. Do not apply heat in the first 48 hours — it can increase swelling.
Head elevation:
Keeping your head elevated — even during sleep — reduces the amount of fluid that pools in the facial tissue. Sleep with an extra pillow for the first two to three nights.
Anti-inflammatory medication:
Anti-inflammatory medications (ibuprofen-based, unless contraindicated) work on the underlying tissue response, not just the pain signal. Taking them as directed — starting before the anaesthetic fully wears off on the day of surgery — can make a meaningful difference to your swelling and recovery.
Always check with your pharmacist or GP before starting anti-inflammatory medication, particularly if you have existing medical conditions.
Stay hydrated:
Adequate hydration supports every aspect of healing. Drink water regularly throughout the recovery period. Avoid alcohol, which can interfere with both healing and medication.
Rest:
It sounds simple, but it’s effective. Rest reduces the metabolic demands on the body, freeing energy for the repair process. Avoid strenuous activity for at least the first 48 hours, and ideally for 72–96 hours.
Avoid smoking:
Smoking dramatically increases the risk of dry socket (by disrupting the blood clot) and slows overall healing. If you smoke, please attempt to abstain for at least 72 hours after your extraction — ideally longer.
Foods That Help vs Foods That Make Swelling Worse
Your diet has a real impact on how your body manages inflammation during recovery.
Foods That Support Recovery
- Soft, nutrient-dense foods: Eggs, yoghurt, soft fish, mashed vegetables, smooth soups, porridge, avocado
- Cold foods for the first 24 hours: Cold (not icy) yoghurt, cool smoothies, lukewarm soups — the cooler temperature has a mild anti-inflammatory effect on the tissue
- Foods rich in vitamin C: Smoothies with berries, puréed kiwi or mango (seedless), soft stewed fruit — vitamin C supports tissue repair
- Protein-rich foods: Adequate protein intake supports healing. Eggs, soft legumes, yoghurt, and soft tofu are all easy options
- Broths and soups: Nourishing, easy to consume, and hydrating
Foods and Habits That Can Worsen Swelling or Slow Healing
- Hard, crunchy, or chewy foods: Seeds, nuts, crusty bread, raw vegetables, chips — these can dislodge the clot or irritate the socket
- Very hot foods or drinks: Heat to the area increases blood flow and can worsen swelling in the first 24–48 hours. Let hot drinks cool before consuming.
- Alcohol: Interferes with healing and can interact with pain relief medications. Avoid for at least 48 hours, preferably longer.
- Spicy foods: Can irritate the healing socket tissue
- Straws and smoking: The suction involved in using straws or smoking can dislodge the blood clot — a leading cause of dry socket. Avoid both for at least 72 hours.
When to Contact Karrinyup Dental Centre About Your Swelling
We encourage all our patients to contact us if they’re unsure about anything during their recovery. It’s always better to ask.
Please call us if:
- Your swelling is increasing after Day 3, rather than improving
- You develop a fever (above 38°C) alongside your dental symptoms
- You experience a sudden increase in pain after a period of improvement (possible dry socket)
- You notice swelling spreading toward your neck, throat, or under your eye
- You have difficulty swallowing, breathing, or opening your mouth
- You’re concerned — there’s no threshold of "too small a worry" when it comes to your health
For follow-up concerns after an extraction, you can also visit our Wisdom Teeth Removal page for more information, or our Emergency Dentist page if you’re experiencing urgent symptoms.
You may also find our post "A Week-by-Week Guide to Wisdom Teeth Surgery Recovery" helpful — it covers the full recovery window in more detail.
And for any general questions about your dental health after your procedure, our General Dentistry team is always available.
Frequently Asked Questions
How long does swelling last after wisdom tooth extraction?
For most patients, swelling after wisdom tooth extraction peaks at around 48 to 72 hours after the procedure, then gradually reduces over the following days. By Day 5 to 7, most patients notice a significant improvement, and the face typically looks close to normal by the end of the first week to ten days. The exact timeline varies depending on the complexity of the extraction, the position of the tooth, and individual healing response. Upper wisdom tooth extractions tend to produce less noticeable swelling than lower ones. Recovery varies — if your swelling is not improving after Day 3, please contact us.
Is swelling worse on Day 3?
Swelling typically peaks between 48 and 72 hours after the extraction — which for many patients corresponds to Day 2 or Day 3. This often surprises patients who expected to feel progressively better from the moment they left the dental chair. If you notice your face looks noticeably puffier on Day 2 or 3 than it did immediately after the procedure, this is usually a normal part of the post-operative process. What’s not normal is swelling that continues to increase after Day 3 without any sign of improvement, or swelling accompanied by fever. If you’re concerned about the degree of your swelling at any stage, please give us a call — we would rather you reach out and hear that everything looks normal than suffer unnecessary worry at home.
What reduces wisdom tooth swelling fastest?
The most effective combination for reducing post-extraction swelling is: cold packs in the first 24–48 hours (20 minutes on, 20 minutes off), head elevation during rest and sleep, anti-inflammatory medication as directed by your dentist or pharmacist, switching to gentle warmth after 48 hours to promote circulation, and adequate rest. None of these alone will eliminate swelling — swelling is a necessary part of healing — but together they can meaningfully reduce its severity and help it resolve more quickly. Individual results vary, and the complexity of your extraction plays a significant role in how much swelling occurs regardless of post-operative care.
Concerned About Your Recovery? We’re Here.
If you’ve recently had wisdom teeth removed at Karrinyup Dental Centre and you have questions about your recovery, please reach out. Our team is here to support you through the full healing process — not just during the appointment.
Dr Justin Soon and the Karrinyup Dental Centre team have been supporting patients through wisdom tooth extractions and recovery for more than 20 years. We know the recovery process can feel unpredictable, and we’re always happy to answer questions and provide reassurance when you need it.
Book a follow-up appointment or reach out with any concerns at karrinyupdental.com.au.
Sources
- Australian Dental Association (ADA) — Post-operative care guidelines for third molar extractions
- Dental Health Services Victoria — Patient information: wisdom teeth removal and recovery
- National Health and Medical Research Council (NHMRC) — Guidelines on management of complications post-dental extraction