If you’ve been waking up with a dull, persistent ache around your jaw — or you’ve noticed pain radiating into your ear, neck, or even your head — you may be wondering whether your wisdom teeth are to blame.
It’s a question we hear regularly at Karrinyup Dental Centre. And the honest answer is: yes, wisdom teeth can absolutely cause jaw pain. But because jaw pain has many possible causes, it’s important to have a proper examination before assuming the culprit.
This article explains how wisdom teeth develop, why they so often cause problems, what wisdom tooth jaw pain typically feels like, and when you should treat your symptoms as a dental emergency. If you’re in Karrinyup or the surrounding suburbs and you’re concerned about jaw pain, we hope this gives you the clarity you need.
Disclaimer: If you are currently experiencing jaw pain, do not rely on this article for a clinical diagnosis. Please book an appointment so we can properly assess what’s happening.
Contents Navigation
- How Wisdom Teeth Develop and Erupt
- Why Wisdom Teeth Cause Jaw Pain
- What Does Wisdom Tooth Jaw Pain Feel Like?
- When Is Jaw Pain a Dental Emergency?
- How Karrinyup Dental Centre Diagnoses Wisdom Tooth Problems
- Treatment Options for Wisdom Tooth Jaw Pain
- Frequently Asked Questions
- Book an Appointment at Karrinyup Dental Centre
- Sources
How Wisdom Teeth Develop and Erupt
Wisdom teeth — formally known as third molars — are the last teeth to develop in the human mouth. Most people have four of them, one in each corner of the jaw. They typically begin forming in the teenage years and attempt to erupt (push through the gumline) sometime between the ages of 17 and 25, though this can vary considerably.
The timing itself isn’t the problem. The problem is space.
By the time wisdom teeth are ready to emerge, the rest of your adult teeth are firmly established. For many people, there simply isn’t enough room at the back of the jaw to accommodate four large new teeth. When space runs out, wisdom teeth can become impacted — meaning they’re unable to fully emerge and instead become trapped beneath the gum, angled against neighbouring teeth, or only partially visible above the gumline.
According to current dental practice guidelines in Australia, impacted wisdom teeth are one of the most common reasons people aged 17 to 35 present to a dentist with unexplained jaw or facial pain.
There are several ways a wisdom tooth can become impacted:
- Mesial impaction — the tooth angles forward toward the front of the mouth (the most common type)
- Distal impaction — the tooth angles backward toward the back of the jaw
- Vertical impaction — the tooth grows straight down but lacks space to erupt fully
- Horizontal impaction — the tooth grows sideways, directly into the roots of the adjacent molar
Each of these presentations can cause pain, but some are more likely to become urgent problems than others.
Why Wisdom Teeth Cause Jaw Pain
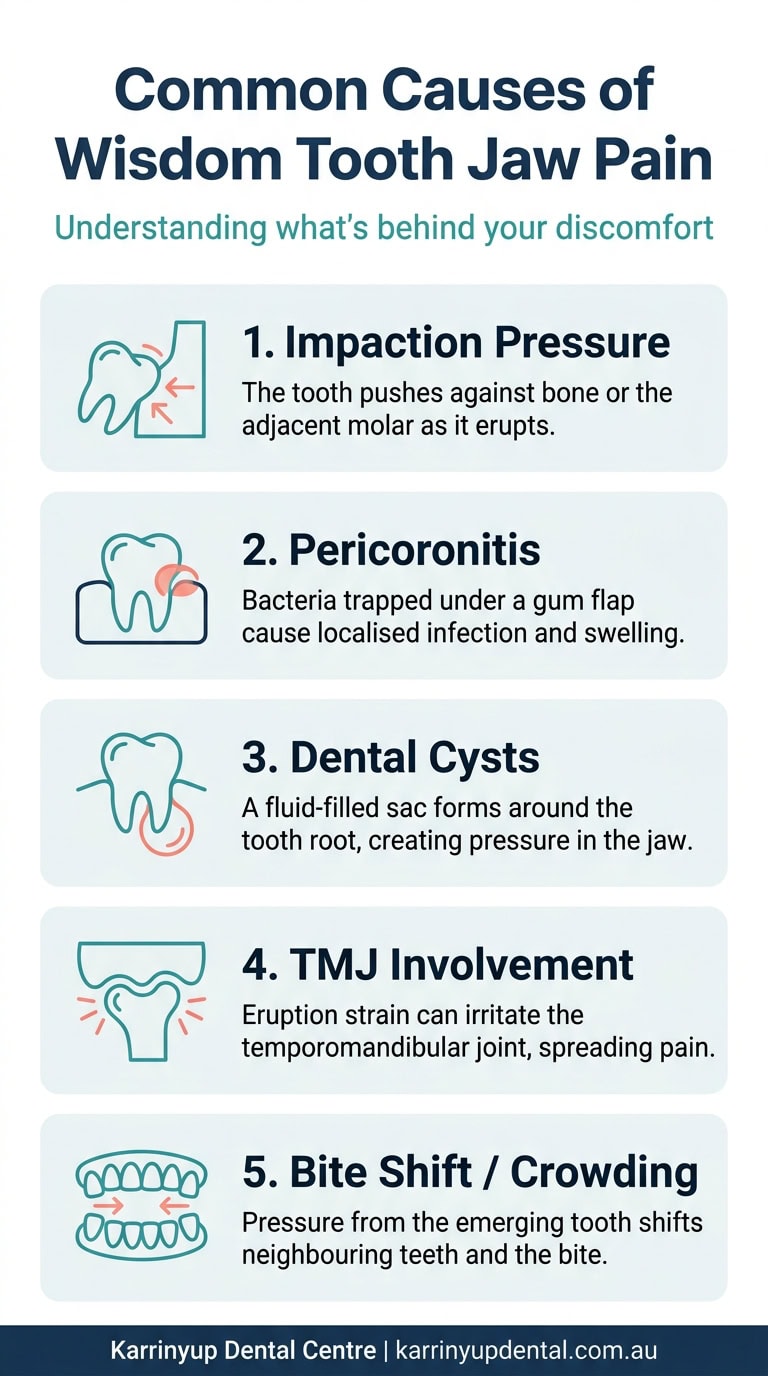
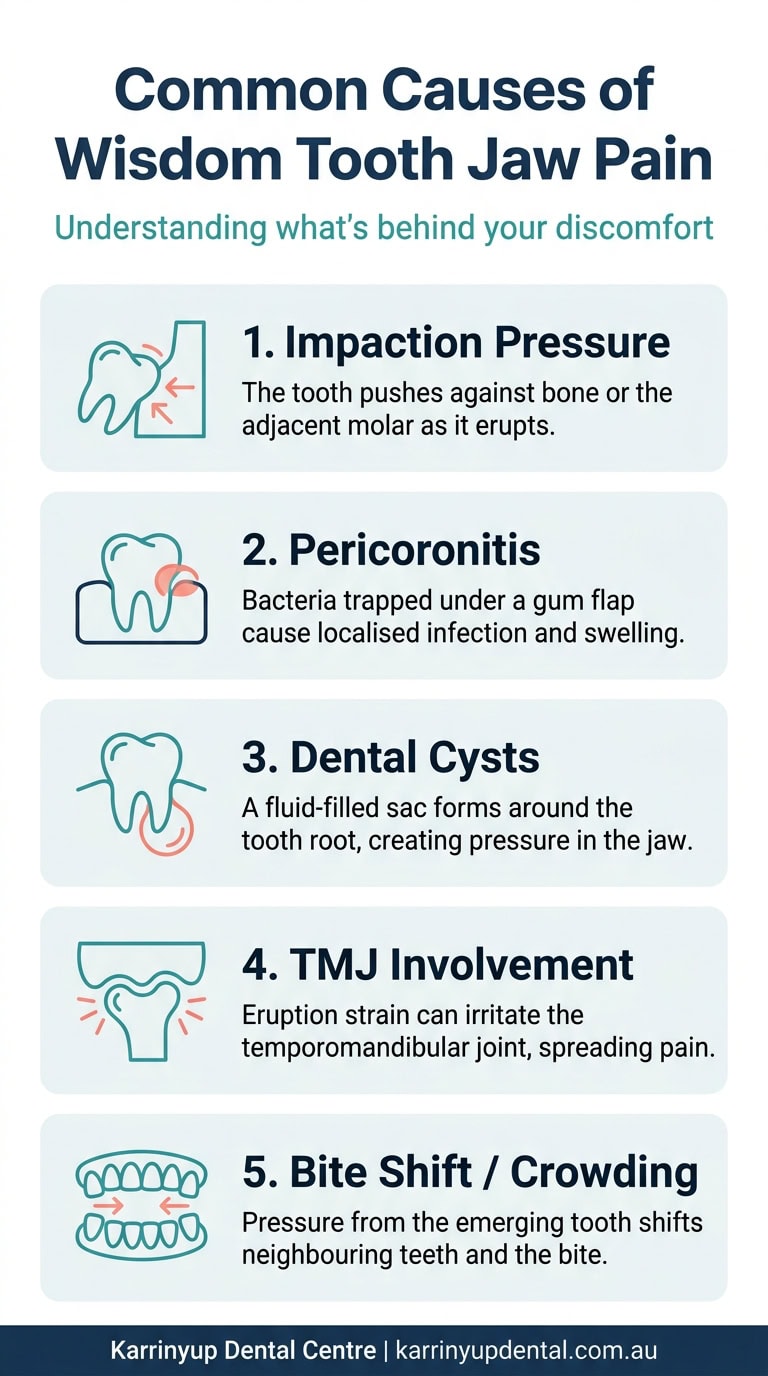
There are several distinct mechanisms through which wisdom teeth can create jaw pain. Understanding which one applies to your situation helps your dentist plan the right treatment.
1. Pressure From Impaction
When a wisdom tooth is angled or trapped beneath the gum, it doesn’t stop growing. It continues to push — and that pressure has nowhere to go except into the surrounding bone, gum tissue, and neighbouring teeth. The result is a deep, constant ache that often feels like it’s coming from somewhere inside the jaw rather than the tooth surface itself.
This pressure can also cause your second molar (the tooth directly in front of the wisdom tooth) to shift or become sore. In some cases, patients notice their lower front teeth beginning to crowd — a sign that wisdom tooth pressure has created a chain reaction across the dental arch.
2. Pericoronitis — Infection Under the Gum Flap
This is one of the most common causes of acute wisdom tooth jaw pain, particularly with lower wisdom teeth.
When a wisdom tooth only partially erupts, a flap of gum tissue typically covers part of the tooth. That flap is extremely difficult to keep clean. Food debris and bacteria accumulate underneath it, creating the ideal conditions for a localised infection called pericoronitis.
Pericoronitis causes:
- Intense throbbing pain around the back of the jaw
- Swollen, red, and tender gum tissue
- A bad taste or smell in the mouth
- Difficulty fully opening the mouth (trismus)
- Pain that radiates into the throat, ear, or neck
In mild cases, pericoronitis can be managed with a professional clean and antiseptic rinse. In more severe cases, antibiotics may be required before the tooth can safely be removed.
3. Dental Cysts and Follicular Growths
Less commonly, a fluid-filled sac called a dentigerous cyst can form around the crown of an impacted wisdom tooth. These cysts develop from tissue that surrounds the developing tooth and can grow slowly over months or years without causing obvious symptoms — until they become large enough to press on surrounding bone and nerves.
Cysts associated with impacted wisdom teeth can cause:
- A persistent, deep jaw ache
- Visible swelling along the jawline
- Loosening of nearby teeth
- Numbness in the lower lip or chin (if the inferior alveolar nerve is involved)
This is one of the reasons dentists recommend monitoring impacted wisdom teeth with periodic X-rays, even when they’re not currently causing pain. Cysts caught early are far easier to manage.
4. Temporomandibular Joint (TMJ) Involvement
The temporomandibular joints are the hinges that connect your lower jaw to your skull, located just in front of each ear. Wisdom tooth problems — particularly pericoronitis or impaction-related pain — can cause patients to unconsciously alter how they chew, clench, or hold their jaw. Over time, this compensatory behaviour can irritate or strain the TMJ.
The result is a complex presentation: wisdom tooth-related jaw pain that has spread to involve the jaw joint itself, creating clicking, locking, headaches, and ear pain that outlasts the original dental problem.
5. Crowding and Bite Shift
Even wisdom teeth that partially erupt without infection can apply subtle, sustained pressure on the dental arch. This can shift how upper and lower teeth meet when you bite down. When the bite changes, the jaw muscles work harder to find a comfortable position — and that muscle overwork is a common source of jaw aching, particularly noticeable in the mornings.
What Does Wisdom Tooth Jaw Pain Feel Like?
Wisdom tooth jaw pain is not always easy to distinguish from other causes of jaw pain, which is exactly why professional assessment matters. That said, there are some common patterns worth knowing.
Common symptoms associated with wisdom tooth jaw pain:
- A dull, persistent ache at the very back of the jaw that may be worse when chewing
- Soreness or swelling in the gum tissue behind the last visible molar
- Pain that seems to radiate into the ear, neck, or temple
- Intermittent sharp pain when biting down
- Difficulty opening the mouth fully, particularly in the morning
- A bad taste at the back of the mouth, especially after eating
- Tenderness when pressing on the angle of the jaw from the outside
Symptoms that are less likely to be wisdom tooth-related:
- Pain primarily in the jaw joint itself (directly in front of the ear)
- Clicking or popping sounds when opening or closing the mouth, without back-of-jaw pain
- Pain that’s worst when you’re stressed or during teeth-grinding episodes
- Pain distributed evenly across the jaw rather than concentrated at the back
That said, as noted above, these categories overlap significantly. Wisdom tooth problems can trigger TMJ problems, and existing TMJ issues can be worsened by wisdom tooth eruption. A proper examination is the only reliable way to understand what’s driving your symptoms.
When Is Jaw Pain a Dental Emergency?

Not all wisdom tooth pain requires an emergency appointment, but certain symptoms should prompt you to seek care urgently.
See a dentist as soon as possible if you experience:
- Rapidly increasing swelling in the jaw, cheek, or neck
- Difficulty swallowing or breathing
- A high fever alongside jaw pain
- Trismus — the inability to open your mouth more than 20–25 mm
- Pain that is not responding to over-the-counter pain relief
- Swelling that is extending toward the eye socket or down into the neck
- Feeling generally unwell alongside localised jaw pain
These symptoms may indicate a spreading dental infection. Dental infections, if left untreated, can spread into the fascial spaces of the face and neck — a serious condition that requires prompt medical attention.
For urgent dental situations in Karrinyup and surrounding suburbs, you can contact Karrinyup Dental Centre directly. We make every effort to accommodate patients experiencing acute dental pain. You can also visit our Emergency Dentist page for more information on how we handle urgent presentations.
How Karrinyup Dental Centre Diagnoses Wisdom Tooth Problems
When you come in with jaw pain that may be related to your wisdom teeth, we don’t just look at the back of your mouth and make a judgement call. A thorough assessment typically includes:
Clinical examination: We assess the gum tissue around your wisdom teeth, check for signs of pericoronitis (redness, swelling, discharge), evaluate how far each tooth has erupted, and test whether neighbouring teeth are tender or have shifted.
Digital X-rays: A periapical or panoramic X-ray gives us a full picture of where your wisdom teeth are positioned, how they’re angled, and whether any cysts or bone changes are present. Panoramic (OPG) X-rays are particularly useful because they show all four wisdom teeth simultaneously alongside the surrounding structures, including the inferior alveolar nerve canal.
Bite and TMJ assessment: If your jaw symptoms suggest possible joint involvement, we’ll also assess your bite, jaw opening range, and joint sounds to determine whether there’s a TMJ component that needs to be addressed alongside (or independently of) the wisdom tooth issue.
Medical history review: Some systemic conditions and medications can influence how wisdom tooth problems present and how they should be managed. We take this context into account.
Once we have a complete picture, we can give you an honest, evidence-based recommendation — whether that’s monitoring with regular X-rays, a conservative clean and rinse, antibiotics, or extraction.
Treatment Options for Wisdom Tooth Jaw Pain
There is no single treatment that applies to all presentations of wisdom tooth jaw pain. The right approach depends on what’s causing the pain, how severe it is, and the specific position and condition of the tooth. Here are the most common management paths.
Monitoring
If a wisdom tooth is fully erupted, in good alignment, not infected, and not causing crowding, monitoring may be appropriate — particularly for younger patients whose wisdom teeth are still erupting and may settle into a functional position.
Monitoring involves regular dental reviews and periodic X-rays to check that no changes are occurring. It is not a passive "do nothing" approach — it requires consistent follow-through.
Professional Cleaning and Antiseptic Irrigation
For mild pericoronitis where the infection is localised, a professional clean of the area under the gum flap — combined with antiseptic irrigation — can resolve the acute episode. This is often followed by a course of antiseptic mouthwash and a recommendation to monitor or plan extraction before the next episode.
Note: Pericoronitis has a high recurrence rate if the underlying tooth is not removed. Many patients experience two or three episodes of pericoronitis before opting for tooth extraction.
Antibiotics
Antibiotics may be prescribed if a pericoronitis infection has spread beyond the immediate gum tissue, if there are signs of systemic involvement (swollen lymph nodes, fever), or as a pre-extraction measure when active infection is present.
It’s important to understand that antibiotics treat the infection — they do not resolve the underlying problem. Once the antibiotic course is finished and the acute infection has cleared, extraction planning should follow.
Wisdom Tooth Extraction
For most impacted or problematic wisdom teeth, extraction is the definitive treatment. The complexity of the extraction depends on the tooth’s position, depth, and root anatomy.
At Karrinyup Dental Centre, wisdom tooth extractions are performed under local anaesthesia. For patients who experience significant anxiety, we also offer options to help manage discomfort throughout the procedure. Our team will explain what to expect in detail before the appointment so you feel fully prepared.
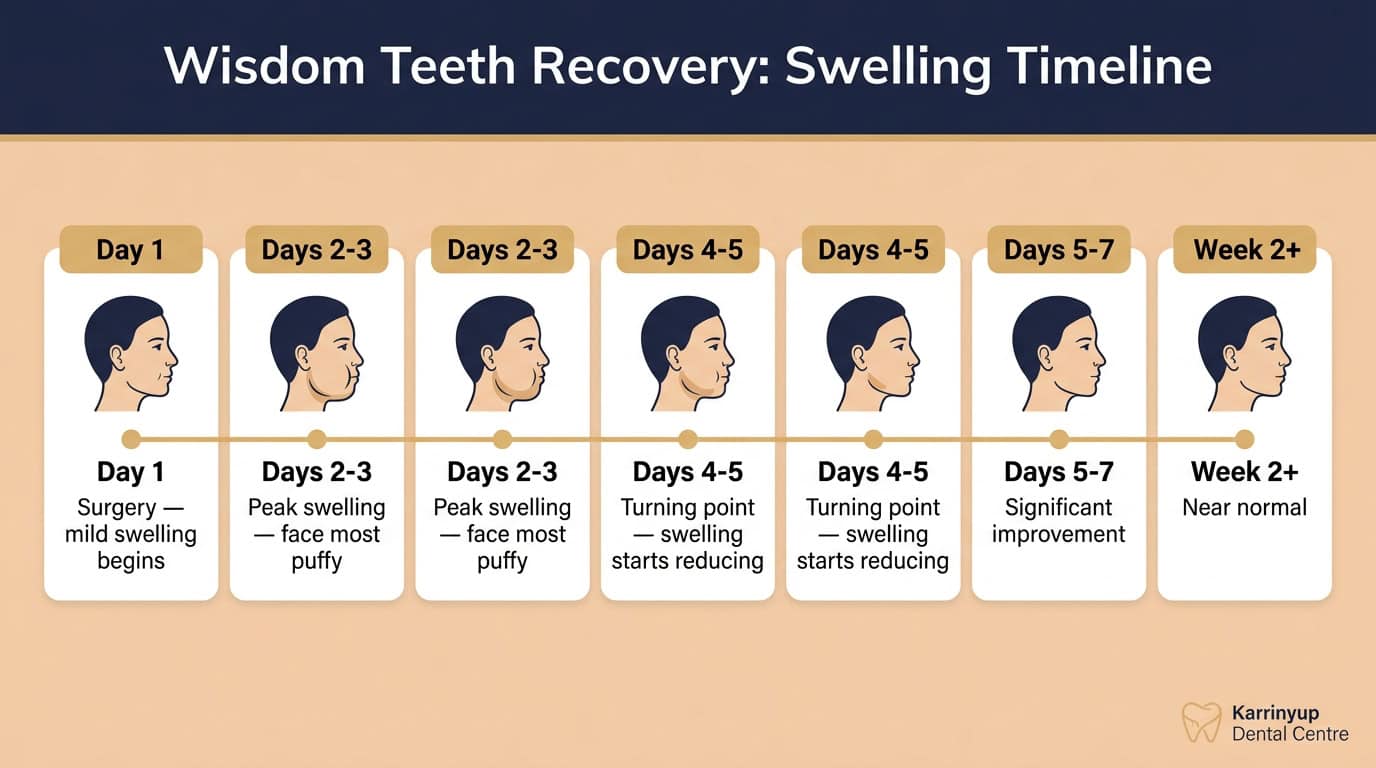
Recovery after wisdom tooth extraction typically involves some swelling and soreness for several days, with most patients returning to normal activities within a week. We provide post-operative care instructions and are available to answer questions during your recovery.
For more information, visit our Wisdom Teeth Removal and General Dentistry pages.
Frequently Asked Questions
Can wisdom teeth cause jaw pain even if they haven’t fully come through?
Yes — in fact, partially erupted wisdom teeth are often more likely to cause jaw pain than fully emerged ones. When a tooth is only partially through the gumline, it creates a pocket where bacteria accumulate, increasing the risk of pericoronitis (gum infection). The pressure from an impacted tooth pushing against bone and neighbouring teeth can also cause significant jaw aching even when the tooth isn’t visible. If you’re experiencing back-of-jaw pain and haven’t had your wisdom teeth assessed recently, it’s worth booking an appointment.
Can wisdom teeth cause ear pain?
Yes, this is a common symptom that surprises many patients. The lower wisdom teeth sit very close to nerves that also serve the ear region. When a wisdom tooth becomes infected or impacted, the referred pain can present in the ear — sometimes feeling exactly like an ear infection. If you’ve seen a GP about ear pain and no ear-related cause was found, it may be worth having your wisdom teeth examined. Jaw pain, ear pain, and headache presenting together are a recognised pattern associated with lower wisdom tooth problems.
Can wisdom teeth cause headaches?
Wisdom teeth can contribute to headaches, though the mechanism is usually indirect. When a wisdom tooth causes jaw pain or forces you to change how you chew or hold your mouth, this can increase tension in the jaw muscles — including the temporalis muscle, which runs along the temple. Sustained muscle tension in this region can produce tension-type headaches. Additionally, if a wisdom tooth problem disrupts sleep, the associated fatigue and muscle clenching can worsen existing headache patterns. Headache alone is rarely sufficient to diagnose a wisdom tooth problem — it should be assessed alongside other jaw and dental symptoms.
Book an Appointment at Karrinyup Dental Centre
If you’re in Karrinyup or the surrounding suburbs and you’ve been dealing with jaw pain that won’t settle, don’t wait for it to become a larger problem.
At Karrinyup Dental Centre, Dr Justin Soon and our experienced team can assess your wisdom teeth thoroughly — with digital X-rays and a clinical examination — and give you a clear, honest picture of what’s happening and what your options are.
We’ve been caring for patients in the Karrinyup community for more than 20 years, and we understand that dental concerns can feel daunting. Our goal is to make your appointment as straightforward and comfortable as possible.
Book your appointment online at karrinyupdental.com.au or call us to arrange a time that suits you.
Sources
- Australian Dental Association (ADA) — Clinical guidelines for assessment and management of impacted third molars
- Dental Health Services Victoria — Patient information on wisdom teeth and pericoronitis
- National Health and Medical Research Council (NHMRC) — Australian guidelines on dental infection management